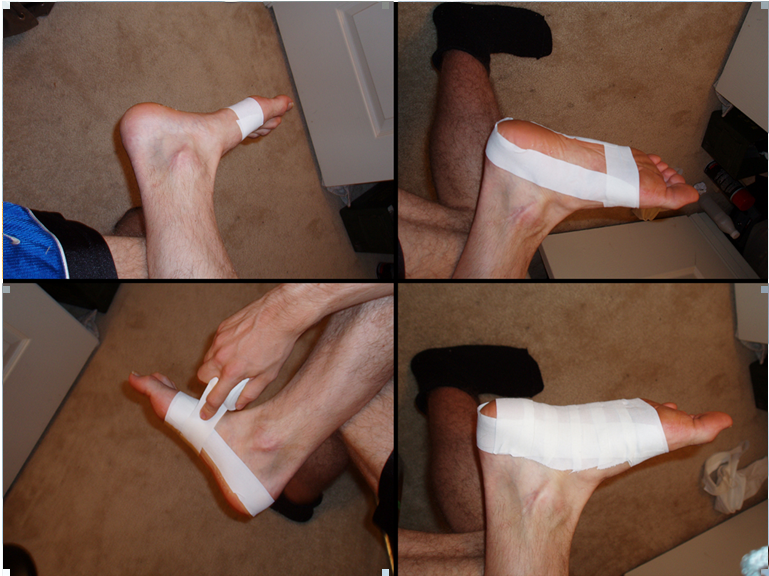
What's The Major Cause Of Achilles Tendonitis ?
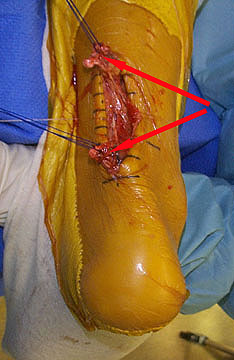 Achilles tendonitis is an iInflammation in the tendon of the calf muscle, where it attaches to the heel bone. Achilles tendonitis causes pain and stiffness at the back of the leg, near the heel. Achilles tendonitis can be caused by overuse of the Achilles tendon, overly tight calf muscles or Achilles tendons, excess uphill running, a sudden increase in the intensity of training or the type of shoes worn to run, or wearing high heels at work and then switching to a lower-heeled workout shoe. Achilles tendonitis causes pain, tenderness, and often swelling over the Achilles tendon. There is pain on rising up on the toes and pain with stretching of the tendon. The range of motion of the ankle may be limited. Treatment includes applying ice packs to the Achilles tendon, raising the lower leg, and taking an anti-inflammatory medication. In some severe cases of Achilles tendonitis, a cast may be needed for several weeks. A heel lift insert may also be used in shoes to prevent future overstretching of the Achilles tendon. Exerting rapid stress on the Achilles tendon when it is inflamed can result in rupture of the tendon.
Achilles tendonitis is an iInflammation in the tendon of the calf muscle, where it attaches to the heel bone. Achilles tendonitis causes pain and stiffness at the back of the leg, near the heel. Achilles tendonitis can be caused by overuse of the Achilles tendon, overly tight calf muscles or Achilles tendons, excess uphill running, a sudden increase in the intensity of training or the type of shoes worn to run, or wearing high heels at work and then switching to a lower-heeled workout shoe. Achilles tendonitis causes pain, tenderness, and often swelling over the Achilles tendon. There is pain on rising up on the toes and pain with stretching of the tendon. The range of motion of the ankle may be limited. Treatment includes applying ice packs to the Achilles tendon, raising the lower leg, and taking an anti-inflammatory medication. In some severe cases of Achilles tendonitis, a cast may be needed for several weeks. A heel lift insert may also be used in shoes to prevent future overstretching of the Achilles tendon. Exerting rapid stress on the Achilles tendon when it is inflamed can result in rupture of the tendon.
Causes
Hill running or stair climbing. Overuse resulting from the natural lack of flexibility in the calf muscles. Rapidly increasing mileage or speed. Starting up too quickly after a layoff. Trauma caused by sudden and hard contraction of the calf muscles when putting out extra effort such as in a final sprint. Achilles tendinitis often begins with mild pain after exercise or running that gradually worsens.
Symptoms
Common symptoms of Achilles tendinitis include, pain and stiffness along the Achilles tendon in the morning, pain along the tendon or back of the heel that worsens with activity, Severe pain the day after exercising, thickening of the tendon, bone spur (insertional tendinitis) swelling that is present all the time and gets worse throughout the day with activity, If you have experienced a sudden "pop" in the back of your calf or heel, you may have ruptured (torn) your Achilles tendon. See your doctor immediately if you think you may have torn your tendon.
Diagnosis
The diagnosis is made via discussion with your doctor and physical examination. Typically, imaging studies are not needed to make the diagnosis. However, in some cases, an ultrasound is useful in looking for evidence of degenerative changes in the tendon and to rule out tendon rupture. An MRI can be used for similar purposes, as well. Your physician will determine whether or not further studies are necessary.
Nonsurgical Treatment
To help heal your Achille?s Tendinitis, follow the R.I.C.E. Principle including Rest, Ice Compression and Elevation. In addition your physiotherapist will likely recommend specific exercises promote healing and strengthening of the Achilles tendon and its supporting structures. As well an orthotic that elevates your heel can reduce stress on your Achilles tendon. Reducing inflammation in the tendon is important too this can often be achieved with oral pills or topical creams. Over-the-counter pain medications or prescription strength such as ibuprofen. However, these drugs can have side effects, like an increased risk of bleeding ulcers. They should be used only occasionally unless your doctor specifically says otherwise. Topical anti-inflammatory creams made with natural ingredients designed specifically for feet and legs (eg ZAX?s Original Heelspur Cream ) target the affected areas and provides effective and safe relief. Tendinitis usually responds well to self-care measures. But if your signs and symptoms are severe or persistent, your doctor might suggest other treatment options including surgery.

Surgical Treatment
Histological and biological studies on tendon healing have made it possible to envisage surgical repair using a percutaneous approach, with the following objectives, a minimal, and not very aggressive, operation, which is quick and easy and within the capabilities of all surgeons, the shortest hospitalisation period possible, above all, early and effective re-education, providing a satisfactory result both in terms of solidity and the comfort of the patient. The percutaneous tenosynthesis TENOLIG combines stability, reliability, patient comfort and lower overall social and professional costs for this type of lesion.
Prevention
If you're just getting started with your training, be sure to stretch after running, and start slowly, increasing your mileage by no more than 10% per week. Strengthen your calf muscles with exercises such as toe raises. Work low-impact cross-training activities, such as cycling and swimming, into your training.
What Is Painful Heel

Overview
Plantar fasciitis is a very common condition resulting in pain under the heel which often radiates into the foot. We explain free of charge everything you need to know to cure your pain and prevent it from returning.
Causes
You are more likely to develop plantar fasciitis if you are Active, sports that place excessive stress on the heel bone and attached tissue, especially if you have tight calf muscles or a stiff ankle from a previous ankle sprain, which limits ankle movement eg. Running, ballet dancing and aerobics. Overweight. Carrying around extra weight increases the strain and stress on your plantar fascia. Pregnant. The weight gain and swelling associated with pregnancy can cause ligaments to become more relaxed, which can lead to mechanical problems and inflammation. On your feet. Having a job that requires a lot of walking or standing on hard surfaces ie factory workers, teachers and waitresses. Flat Feet or High Foot Arches. Changes in the arch of your foot changes the shock absorption ability and can stretch and strain the plantar fascia, which then has to absorb the additional force. Middle-Aged or Older. With ageing the arch of your foot may begin to sag - putting extra stress on the plantar fascia. Wearing shoes with poor support. Weak Foot Arch Muscles. Muscle fatigue allows your plantar fascia to overstress and cause injury. Arthritis. Some types of arthritis can cause inflammation in the tendons in the bottom of your foot, which may lead to plantar fasciitis. Diabetes. Although doctors don't know why, plantar fasciitis occurs more often in people with diabetes.
Symptoms
Plantar fasciitis sufferers feel a sharp stab or deep ache in the middle of the heel or along the arch. Another sign is the morning hobble from the foot trying to heal itself in a contracted position overnight. Taking that first step causes sudden strain on the bottom of the foot. The pain can recur after long spells of sitting, but it tends to fade during a run, once the area is warmed up.
Diagnosis
To diagnose plantar fasciitis, your doctor will physically examine your foot by testing your reflexes, balance, coordination, muscle strength, and muscle tone. Your doctor may also advise a magnetic resonance imaging (MRI) or X-ray to rule out other others sources of your pain, such as a pinched nerve, stress fracture, or bone spur.
Non Surgical Treatment
Reducing inflammation in the plantar fascia ligament is an important part of treatment, though this does not address the underlying damage to the ligament. Initial home treatment includes staying off your feet and applying ice for 15 to 20 minutes three or four times a day to reduce swelling. You can also try reducing or changing your exercise activities. Using arch supports in your shoes and doing stretching exercises may also help to relieve pain. Nonsteroidal anti-inflammatory drugs (NSAIDS), such as ibuprofen (i.e. Motrin or Advil) and naproxen (i.e. Aleve), are often used to reduce inflammation in the ligament. If home treatments and over-the-counter anti-inflammatory drugs don’t ease the pain, an injection of a corticosteroid directly into the damaged section of the ligament can be given. Your doctor can do this in his or her office. Your doctor may use an ultrasound device to help determine the best place for the injection. Corticosteroids can also be administered on the skin of your heel or the arch of your foot, and then a painless electrical current is applied to let the steroid pass through your skin and into the muscle. Physical therapy is an important part of treatment for planter fasciitis. It can help stretch your plantar fascia and Achilles tendons. A physical therapist can also show you exercises to strengthen your lower leg muscles, helping to stabilize your walk and lessen the workload on your plantar fascia. If pain continues and other methods aren’t working, your doctor may recommend extracorporeal shock wave therapy. Sound waves are bombarded against your heel to stimulate healing within the ligament. This treatment can result in bruises, swelling, pain, and numbness, and has not been proven to be consistently effective in relieving symptoms.

Surgical Treatment
Surgery should be reserved for patients who have made every effort to fully participate in conservative treatments, but continue to have pain from plantar fasciitis. Patients should fit the following criteria. Symptoms for at least 9 months of treatment. Participation in daily treatments (exercises, stretches, etc.). If you fit these criteria, then surgery may be an option in the treatment of your plantar fasciitis. Unfortunately, surgery for treatment of plantar fasciitis is not as predictable as a surgeon might like. For example, surgeons can reliably predict that patients with severe knee arthritis will do well after knee replacement surgery about 95% of the time. Those are very good results. Unfortunately, the same is not true of patients with plantar fasciitis.
Stretching Exercises
Calf stretch. Lean forward against a wall with one knee straight and the heel on the ground. Place the other leg in front, with the knee bent. To stretch the calf muscles and the heel cord, push your hips toward the wall in a controlled fashion. Hold the position for 10 seconds and relax. Repeat this exercise 20 times for each foot. A strong pull in the calf should be felt during the stretch. Plantar fascia stretch. This stretch is performed in the seated position. Cross your affected foot over the knee of your other leg. Grasp the toes of your painful foot and slowly pull them toward you in a controlled fashion. If it is difficult to reach your foot, wrap a towel around your big toe to help pull your toes toward you. Place your other hand along the plantar fascia. The fascia should feel like a tight band along the bottom of your foot when stretched. Hold the stretch for 10 seconds. Repeat it 20 times for each foot. This exercise is best done in the morning before standing or walking.
What Exactly Causes Heel Discomfort

Overview
To find out where this condition gets its name, we need to look at a specific area of the foot. Your foot is made up of bones, muscles, tendons, and ligaments. The plantar fascia is a relatively inflexible, strong, fibrous band on the bottom of the foot that supports the arch of your foot. Beginning at the heel bone, the plantar fascia extends the length of your foot to connect with your toes at the ball of the foot. When you walk, your weight is distributed across your feet. Any imbalances in the mechanics of your foot and distribution of weight can potentially cause pain. Diseases involving inflammation end with "itis." This explains the name of the condition as being an inflammation of the plantar fascia, thus plantar fasciitis. Repetitive movements such as walking or running stretch the plantar fascia. Because it is not very flexible, this can cause small tears in the fascia, which leads to inflammation and pain. Other factors such as high arches, fallen arches, or a change in the walking surface contribute to the stress placed on the plantar fascia and heel.
Causes
Under normal circumstances, your plantar fascia acts like a shock-absorbing bowstring, supporting the arch in your foot. If tension on that bowstring becomes too great, it can create small tears in the fascia. Repetitive stretching and tearing can cause the fascia to become irritated or inflamed.
Symptoms
Among the symptoms for Plantar Fasciitis is pain usually felt on the underside of the heel, often most intense with the first steps after getting out of bed in the morning. It is commonly associated with long periods of weight bearing or sudden changes in weight bearing or activity. Plantar Fasciitis also called “policeman’s heel” is presented by a sharp stabbing pain at the bottom or front of the heel bone. In most cases, heel pain is more severe following periods of inactivity when getting up and then subsides, turning into a dull ache.
Diagnosis
During the physical exam, your doctor checks for points of tenderness in your foot. The location of your pain can help determine its cause. Usually no tests are necessary. The diagnosis is made based on the history and physical examination. Occasionally your doctor may suggest an X-ray or magnetic resonance imaging (MRI) to make sure your pain isn't being caused by another problem, such as a stress fracture or a pinched nerve. Sometimes an X-ray shows a spur of bone projecting forward from the heel bone. In the past, these bone spurs were often blamed for heel pain and removed surgically. But many people who have bone spurs on their heels have no heel pain.
Non Surgical Treatment
Most doctors recommend an initial six- to eight-week program of conservative treatment, including Rest, balanced with stretching exercises to lengthen the heel cord and plantar fascia. Ice massage to the bottom of the foot after activities that trigger heel pain. Avoidance of walking barefoot or wearing slippers or sandals that provide little arch support. A temporary switch to swimming and/or bicycling instead of sports that involve running and jumping. Shoes with soft heels and insoles. Taping the bottom of the injured foot. Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen (Advil, Motrin and other brand names), or acetaminophen (Tylenol) for pain. Physical therapy using ultrasound, electrical stimulation with corticosteroids or massage techniques. If this conservative treatment does not help, your doctor may recommend that you wear a night splint for six to eight weeks. While you sleep, the night splint will keep your foot in a neutral or slightly flexed (bent) position to help maintain the normal stretch of the plantar fascia and heel cord. If the night splint doesn't work, your doctor may inject corticosteroid medication into the painful area or place your foot in a short leg cast for one to three months. Shock wave therapy, in which focused sound energy is applied to the sore heel, may be recommended for plantar fasciitis. The shock waves are intended to irritate or injure the plantar fascia to promote healing. The overall benefit of this approach is uncertain. Other therapies that have been tried include radiation therapy and botulinum toxin injections. But their effectiveness is unclear. If all else fails, your doctor may suggest surgery. But this is rare, and surgery is not always successful.

Surgical Treatment
Surgery for plantar fasciitis can be very successful in the right patients. While there are potential complications, about 70-80% of patients will find relief after plantar fascia release surgery. This may not be perfect, but if plantar fasciitis has been slowing you down for a year or more, it may well be worth these potential risks of surgery. New surgical techniques allow surgery to release the plantar fascia to be performed through small incisions using a tiny camera to locate and cut the plantar fascia. This procedure is called an endoscopic plantar fascia release. Some surgeons are concerned that the endoscopic plantar fascia release procedure increases the risk of damage to the small nerves of the foot. While there is no definitive answer that this endoscopic plantar fascia release is better or worse than a traditional plantar fascia release, most surgeons still prefer the traditional approach.
What Causes Pain In The Heel And The Way To Deal With It

Overview
The plantar fascia is a band of connective tissue that runs along the sole from the heel to the ball of the foot. One of its main roles is to keep the bones and joints in position. Bruising or overstretching this ligament can cause inflammation and heel pain. A common cause is flat feet, because the ligament is forced to overstretch as the foot spreads out and the arch flattens. The pain may be worse first thing in the morning or after rest. In many cases, plantar fasciitis is associated with heel spur. The plantar fascia tears and bleeds at the heel and, over time, these injuries calcify and form a bony growth.
Causes
Plantar fasciitis can be confused with a condition called tarsal tunnel syndrome. In tarsal tunnel syndrome, an important nerve in the foot, the tibial nerve, is trapped and pinched as it passes through the tarsal tunnel, a condition analogous to carpal tunnel syndrome in the wrist. This may cause symptoms similar to the pain of a plantar fasciitis. There are also other less common problems such as nerve entrapments, stress fractures, and fat pad necrosis, all of which can cause foot pain. Finally, several rheumatologic conditions can cause heel pain. These syndromes such as Reiter's syndrome and ankylosing spondylitis can cause heel pain similar to plantar fasciitis. If your symptoms are not typical for plantar fasciitis, or if your symptoms do not resolve with treatment, your doctor will consider these possible diagnoses.
Symptoms
Plantar fasciitis generally occurs in one foot. Bilateral plantar fasciitis is unusual and tends to be the result of a systemic arthritic condition that is exceptionally rare among athletes. Males suffer from a somewhat greater incidence of plantar fasciitis than females, perhaps as a result of greater weight coupled with greater speed and ground impact, as well as less flexibility in the foot. Typically, the sufferer of plantar fasciitis experiences pain upon rising after sleep, particularly the first step out of bed. Such pain is tightly localized at the bony landmark on the anterior medial tubercle of the calcaneus. In some cases, pain may prevent the athlete from walking in a normal heel-toe gait, causing an irregular walk as means of compensation. Less common areas of pain include the forefoot, Achilles tendon, or subtalar joint. After a brief period of walking, the pain usually subsides, but returns again either with vigorous activity or prolonged standing or walking. On the field, an altered gait or abnormal stride pattern, along with pain during running or jumping activities are tell-tale signs of plantar fasciitis and should be given prompt attention. Further indications of the injury include poor dorsiflexion (lifting the forefoot off the ground) due to a shortened gastroc complex, (muscles of the calf). Crouching in a full squat position with the sole of the foot flat on the ground can be used as a test, as pain will preclude it for the athlete suffering from plantar fasciitis, causing an elevation of the heel due to tension in the gastroc complex.
Diagnosis
Plantar fasciitis is usually diagnosed by a health care provider after consideration of a person’s presenting history, risk factors, and clinical examination. Tenderness to palpation along the inner aspect of the heel bone on the sole of the foot may be elicited during the physical examination. The foot may have limited dorsiflexion due to tightness of the calf muscles or the Achilles tendon. Dorsiflexion of the foot may elicit the pain due to stretching of the plantar fascia with this motion. Diagnostic imaging studies are not usually needed to diagnose plantar fasciitis. However, in certain cases a physician may decide imaging studies (such as X-rays, diagnostic ultrasound or MRI) are warranted to rule out other serious causes of foot pain. Bilateral heel pain or heel pain in the context of a systemic illness may indicate a need for a more in-depth diagnostic investigation. Lateral view x-rays of the ankle are the recommended first-line imaging modality to assess for other causes of heel pain such as stress fractures or bone spur development. Plantar fascia aponeurosis thickening at the heel greater than 5 millimeters as demonstrated by ultrasound is consistent with a diagnosis of plantar fasciitis. An incidental finding associated with this condition is a heel spur, a small bony calcification on the calcaneus (heel bone), which can be found in up to 50% of those with plantar fasciitis. In such cases, it is the underlying plantar fasciitis that produces the heel pain, and not the spur itself. The condition is responsible for the creation of the spur though the clinical significance of heel spurs in plantar fasciitis remains unclear.
Non Surgical Treatment
Your GP or podiatrist may advise you to change your footwear. You should avoid wearing flat-soled shoes, because they will not provide your heel with support and could make your heel pain worse. Ideally, you should wear shoes that cushion your heels and provide a good level of support to the arches of your feet. For women wearing high heels, and for men wearing heeled boots or brogues, can provide short- to medium-term pain relief, as they help reduce pressure on the heels. However, these types of shoes may not be suitable in the long term, because they can lead to further episodes of heel pain. Your GP or podiatrist can advise on footwear. Orthoses are insoles that fit inside your shoe to support your foot and help your heel recover. You can buy orthoses off-the-shelf from sports shops and larger pharmacies. Alternatively, your podiatrist should be able to recommend a supplier. If your pain does not respond to treatment and keeps recurring, or if you have an abnormal foot shape or structure, custom-made orthoses are available. These are specifically made to fit the shape of your feet. However, there is currently no evidence to suggest that custom-made orthoses are more effective than those bought off-the-shelf. An alternative to using orthoses is to have your heel strapped with sports strapping (zinc oxide) tape, which helps relieve pressure on your heel. Your GP or podiatrist can teach you how to apply the tape yourself. In some cases, night splints can also be useful. Most people sleep with their toes pointing down, which means tissue inside the heel is squeezed together. Night splints, which look like boots, are designed to keep your toes and feet pointing up while you are asleep. This will stretch both your Achilles tendon and your plantar fascia, which should help speed up your recovery time. Night splints are usually only available from specialist shops and online retailers. Again, your podiatrist should be able to recommend a supplier. If treatment hasn't helped relieve your painful symptoms, your GP may recommend corticosteroid injections. Corticosteroids are a type of medication that have a powerful anti-inflammatory effect. They have to be used sparingly because overuse can cause serious side effects, such as weight gain and high blood pressure (hypertension). As a result, it is usually recommended that no more than three corticosteroid injections are given within a year in any part of the body. Before having a corticosteroid injection, a local anaesthetic may be used to numb your foot so you don't feel any pain.

Surgical Treatment
Surgery is not a common treatment for this condition. Approximately 5% of people with plantar fasciitis require surgery if non-surgical methods do not help to relieve pain within a year. The surgical procedure involves making an incision in the plantar fascia in order to decrease the tension of the ligament. Potential risks of this surgical procedure include irritation of the nerves around the heel, continued plantar fasciitis, heel or foot pain, infection, flattening of the arch, problems relating to the anesthetic.
Prevention
Plantar fasciitis can be a nagging problem, which gets worse and more difficult to treat the longer it's present. To prevent plantar fasciitis, run on soft surfaces, keep mileage increases to less than 10 percent per week, and visit a specialty running shop to make sure you're wearing the proper shoes for your foot type and gait. It's also important to stretch the plantar fascia and Achilles tendon.
What Triggers Heel Discomfort To Appear

Overview
Plantar fasciitis is sometimes mixed up with a heel spur although they are not the same. A heel spur is a calcium deposit that occurs where the plantar fascia is attached to the heel bone (calcaneus). In many cases a heel spur is found on a foot with no pain or other symptoms at all. And in many painful heels there is no sign for a heel spur. Heel spur and painful heal does not necessarily go together. For many years plantar fasciitis was believed to be an inflammatory condition. It is thought now to be inaccurate because there were many cases of the disorder with no inflammatory signs observed within the fascia. The heel pain cause is now believed to be damage to the collagen fibers of the fascia. This damage, caused by stress injury, sometimes may include inflammatory cells.
Causes
This is a problem of either extreme, so people with high arches or those that have very flat feet are at risk of developing pain in this region. This is because of the relative stress the plantar fascia is put under. In people with excessive pronation, the plantar fascia is put under too much stretch, as their range flattens and strains it. People with a stiff, supinated (high-arched) foot lack the flexibility to appropriately shock absorb, so this too puts extra strain on the plantar fascia. Clinically, we see more people presenting with plantar fascia pain who have excessive pronation than those with stiff, supinated feet. But while the foot type is the biggest risk factor for plantar fasciitis, the whole leg from the pelvis down can affect how the foot hits the ground. A thorough biomechanical assessment will determine where in the kinetic chain things have gone wrong to cause the overload.
Symptoms
Plantar fasciitis and heel spur pain usually begins in the bottom of the heel, and frequently radiates into the arch. At times, however, the pain may be felt only in the arch. The pain is most intense when first standing, after any period of rest. Most people with this problem experience their greatest pain in the morning, with the first few steps after sleeping. After several minutes of walking, the pain usually becomes less intense and may disappear completely, only to return later with prolonged walking or standing. If a nerve is irritated due to the swollen plantar fascia, this pain may radiate into the ankle. In the early stages of Plantar Fasciitis and Heel Spurs, the pain will usually subside quickly with getting off of the foot and resting. As the disease progresses, it may take longer periods of time for the pain to subside.
Diagnosis
A physical exam performed in the office along with the diagnostic studies as an x-ray. An MRI may also be required to rule out a stress fracture, or a tear of the plantar fascia. These are conditions that do not normally respond to common plantar fasciitis treatment.
Non Surgical Treatment
Treatment for plantar fasciitis includes medication, physical therapy, shock wave therapy, or surgery. Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and naproxen are used to treat the inflammation and pain of plantar fasciitis, but they won’t cure the condition. Corticosteroids can also be used to ease pain and reduce inflammation. Corticosteroids are applied either as a topical solution in conjunction with a non-painful electric current or through injections to the affected area.

Surgical Treatment
When more-conservative measures aren't working, your doctor might recommend steroid shots. Injecting a type of steroid medication into the tender area can provide temporary pain relief. Multiple injections aren't recommended because they can weaken your plantar fascia and possibly cause it to rupture, as well as shrink the fat pad covering your heel bone. Extracorporeal shock wave therapy. In this procedure, sound waves are directed at the area of heel pain to stimulate healing. It's usually used for chronic plantar fasciitis that hasn't responded to more-conservative treatments. This procedure may cause bruises, swelling, pain, numbness or tingling and has not been shown to be consistently effective. Surgery. Few people need surgery to detach the plantar fascia from the heel bone. It's generally an option only when the pain is severe and all else fails. Side effects include a weakening of the arch in your foot.
Prevention
More than with most sports injuries, a little bit of prevention can go a long way toward keeping you free from plantar fasciitis. Here are some tips to follow. Wear supportive shoes that fit you well. When your shoes start to show wear and can no longer give your feet the support they need, it's time to get a new pair. Runners should stop using their old shoes after about 500 miles of use. Have a trained professional at a specialty running store help you find the right pair for your foot type, and then keep your shoes tied and snug when you wear them. Stay in good shape. By keeping your weight in check, you'll reduce the amount of stress on your feet. Stretch your calves and feet before you exercise or play a sport. Ask an athletic trainer or sports medicine specialist to show you some dynamic stretching exercises. Start any new activity or exercise slowly and increase the duration and intensity of the activity gradually. Don't go out and try to run 10 miles the first time you go for a jog. Build up to that level of exercise gradually. Talk to your doctor about getting heel pads, custom shoe inserts, or orthotics to put in your shoes. Foot supports can help cushion your feet and distribute your weight more evenly. This is especially true for people with high arches or flat feet. Your doctor will be able to tell you if shoe inserts and supports might lower your chances of heel injury.
Physical Exercises For feet Corns
TOE CONDITIONS: Ingrown toenails, blood accumulation under the nail plate (subungual hematoma), corns and calluses are all often seen as a result of playing baseball. It is important that good foot hygiene be practiced with washing between the toes and drying the feet well after bathing. Topical antifungals work well to treat athletes foot. ORTHOPEDIC INJURIES: Most orthopedic baseball foot and ankle injuries are acute or sudden. If an individuals foot or ankle is injured, seek immediate evaluation with one of our doctors. If your athlete has a baseball related injury, call our specialists at Advanced Foot and Ankle Center in McKinney and Prosper Texas at 972-542-2155. However, toe numbness and pain occurring together is one such problem that you cannot afford to ignore. Common symptoms are flat feet knee problems , burning sensation, numbness.
Pain often occurs suddenly and mainly around the undersurface of the heel, although it often spreads to your arch. The condition can be temporary, but may become chronic if you ignore it. Resting usually provides relief, but the pain may return. Heel spurs are bony growths that protrude from the bottom of the heel bone, and they are parallel to the ground. There is a nerve that runs very close to this area and may contribute to the pain which occurs.

Rheumatoid arthritis causes forefoot deformity and often may cause displacement and even dislocation of the metatarsal joints themselves. Morton's Neuroma can also be a source of metarsalgia and is characterized by pain in the forefoot. Sesamoiditis is located on the plantar surface of the foot and will be located near the first metatarsal phalangeal joint.

Bunions are bony lumps that develop on the side of your foot and at the base of your big toe. They're the result of a condition called hallux valgus, which causes your big toe joint to bend towards your other toes and become may also develop a bursa here too, especially if your shoes press against the bunion. Sometimes swellings or bursae on the joints in your feet are also called bunions, but these aren't the same as bunions caused by hallux valgus. Hallux valgus is different to hallux rigidus, which is osteoarthritis of the big toe joint. Hallux rigidus causes your big toe to become stiff and its range of movement is reduced. Symptoms of a bunion can be controlled by choosing shoes with a soft, wide upper to reduce pressure and rubbing on your joint. Toes form hammer or claw shape.
Plantar Fasciitis And Heel Pain
To that end, the first goal of treatment should be to protect the plantar fascia from additional strain while it is injured. While the “-itis” suffix implies that inflammation is the cause of plantar heel pain, new evidence indicates that the real problem is damage and degeneration of the fascial fibers5—icing is always a good idea, but it’s not an excuse to continue to strain the plantar fascia with long runs, hard workouts, or unsupportive shoes. Aggressive rehabilitation, combined with avoiding activities that hurt, are your best chance for a speedy recovery. A good plantar fasciitis taping technique can help the foot get the rest it needs by supporting the plantar fascia. Tape is applied in strips across the plantar fascia taking the stress off the foot which healing to take place. Apply ice or cold therapy to help reduce pain and inflammation. Cold therapy can be applied regularly until symptoms have resolved. Stretching the plantar fascia is an important part of treatment and prevention. Simply reducing pain and inflammation alone is unlikely to result in long term recovery. The plantar fascia tightens up making the origin at the heel more susceptible to stress. Play toe tennis. Stand with your foot on a tennis ball. working from the center of your heel, move the ball down either side of your heel toward the ball of your foot. Massaging your foot in this way relaxes the muscles and tissues in the arch of your foot and spreads the metatarsals, the bones in the ball of your foot. Roll a can for relief. To soothe an aching arch, roll your bare foot over a can of coke concentrate for ten minutes. Wrap the can in a towel so that it doesn’t touch your skin. The massage helps loosen tense tissues, while the cold helps reduce inflammation. The "plantar fascia" is a chord of tissue that runs from the heel to the toes on the bottom of the foot. When this tissue becomes inflamed, pain can develop in the heel and it can be quite severe. This is known as "plantar fasciitis." If you are overweight, pregnant, wear shoes with inadequate support or you participate in sports with a lot of impact to the bottom of your feet, your risk for getting plantar fasciitis goes up. If you do develop it, there are several treatment options that you can utilize. Significance The plantar fascia is a strong, fibrous structure that attaches to the heel bone on the bottom of the foot and runs down to the ball of the foot, or metatarsal heads. Its job is to cover the muscles on the bottom of the foot and help form the arch of the foot. Pain in this area can be progressively debilitating and eventually lead to problems walking and standing. Of all the treatment options, stretching exercises are the most successful. There are a number of exercises to reduce plantar fascistic and offer relaxation and relief from the pain and discomfort associated with the condition. The mechanical structure of your feet and the manner in which the different segments of your feet are linked together and joined with your legs has a major impact on their function and on the development of mechanically caused problems. Merely having "flat feet" won't take the spring out of your step, but having badly functioning feet with poor bone alignment will adversely affect the muscles, ligaments, and tendons and can create a variety of aches and pains. Excess pronation can cause the arch of your foot to stretch excessively with each step. This "hypermobility" may cause other bones to shift and cause other mechanically induced problems. It is advisable to use proper shoes because running or walking involves strenuous movements. You can consult a physiotherapist to know the kind of motion control needed. Running shoes for plantar fasciitis provide special structural support around the heel which is not found in normal running shoes. They also have an inbuilt scientific technique to deal with pain. Some shoes do not have any supplementary devices, but instead, have an inbuilt mechanism in the sole which treats the problem. But, these shoes are very costly with a limited number of designs and styles. Custom rigid orthotics is for patients withserious biomechanical disorders and/or foot deformities. Most people simply suffer from fallen arches (over-pronation) do not require an expensive rigid orthotic. Research has shown that for 80% of people suffering from over-pronation an off-the-shelf pre-made orthotic will provide sufficient correction. Pre-made orthotics is also softer than custom-made's and easier to get used to. Regular cushioning footbeds are only designed to provide a cushioning effect and shock absorption. They may feel comfortable at first however they do not address the biomechanical of over-pronation, as an orthotic does.
The plantar fascia is a strong, fibrous structure that attaches to the heel bone on the bottom of the foot and runs down to the ball of the foot, or metatarsal heads. Its job is to cover the muscles on the bottom of the foot and help form the arch of the foot. Pain in this area can be progressively debilitating and eventually lead to problems walking and standing. Of all the treatment options, stretching exercises are the most successful. There are a number of exercises to reduce plantar fascistic and offer relaxation and relief from the pain and discomfort associated with the condition. The mechanical structure of your feet and the manner in which the different segments of your feet are linked together and joined with your legs has a major impact on their function and on the development of mechanically caused problems. Merely having "flat feet" won't take the spring out of your step, but having badly functioning feet with poor bone alignment will adversely affect the muscles, ligaments, and tendons and can create a variety of aches and pains. Excess pronation can cause the arch of your foot to stretch excessively with each step. This "hypermobility" may cause other bones to shift and cause other mechanically induced problems. It is advisable to use proper shoes because running or walking involves strenuous movements. You can consult a physiotherapist to know the kind of motion control needed. Running shoes for plantar fasciitis provide special structural support around the heel which is not found in normal running shoes. They also have an inbuilt scientific technique to deal with pain. Some shoes do not have any supplementary devices, but instead, have an inbuilt mechanism in the sole which treats the problem. But, these shoes are very costly with a limited number of designs and styles. Custom rigid orthotics is for patients withserious biomechanical disorders and/or foot deformities. Most people simply suffer from fallen arches (over-pronation) do not require an expensive rigid orthotic. Research has shown that for 80% of people suffering from over-pronation an off-the-shelf pre-made orthotic will provide sufficient correction. Pre-made orthotics is also softer than custom-made's and easier to get used to. Regular cushioning footbeds are only designed to provide a cushioning effect and shock absorption. They may feel comfortable at first however they do not address the biomechanical of over-pronation, as an orthotic does.